Student Corner
Tamara McErlain is a second year PhD student on a graduate partnership programme between Queen’s University Belfast (QUB) and the National Cancer Institute (NCI) at the National Institutes of Health in Bethesda, and works under the supervision of Dr Meera Murgai (NCI) and Dr Cristina Branco (QUB), which are both interested in early processes affecting the risk for metastatic breast cancer.

Metastasis accounts for ~75% of breast cancer related deaths and this is a process that can occur only if theenvironment distant from the primary tumor is considered favorable for tumor cell growth. The tissues that allow secondary tumours to form are known as the pre-metastatic niche (Figure 1).
Perivascular cells, are cells that surround and support the function of vascular networks in different tissues, and normally function to regulate blood pressure and vessel permeability. They are also implicated in the development of the pre-metastatic niche. It has been shown that perivascular cells in distant organs become activated by primary tumor derived factors which circulate in the blood from the primary breast tumor. Within the primary tumour, breast cancer cells also interact with non-tumour (stromal) cells, which changes the energetic requirements of the tumour, such as what nutrients and mechanisms fuel its growth. Tamara McErlain
Little is known about metabolic priming of the pre-metastatic niche: how do cancer cells, that migrate from the breast, meet their energy requirements to continue to grow elsewhere?
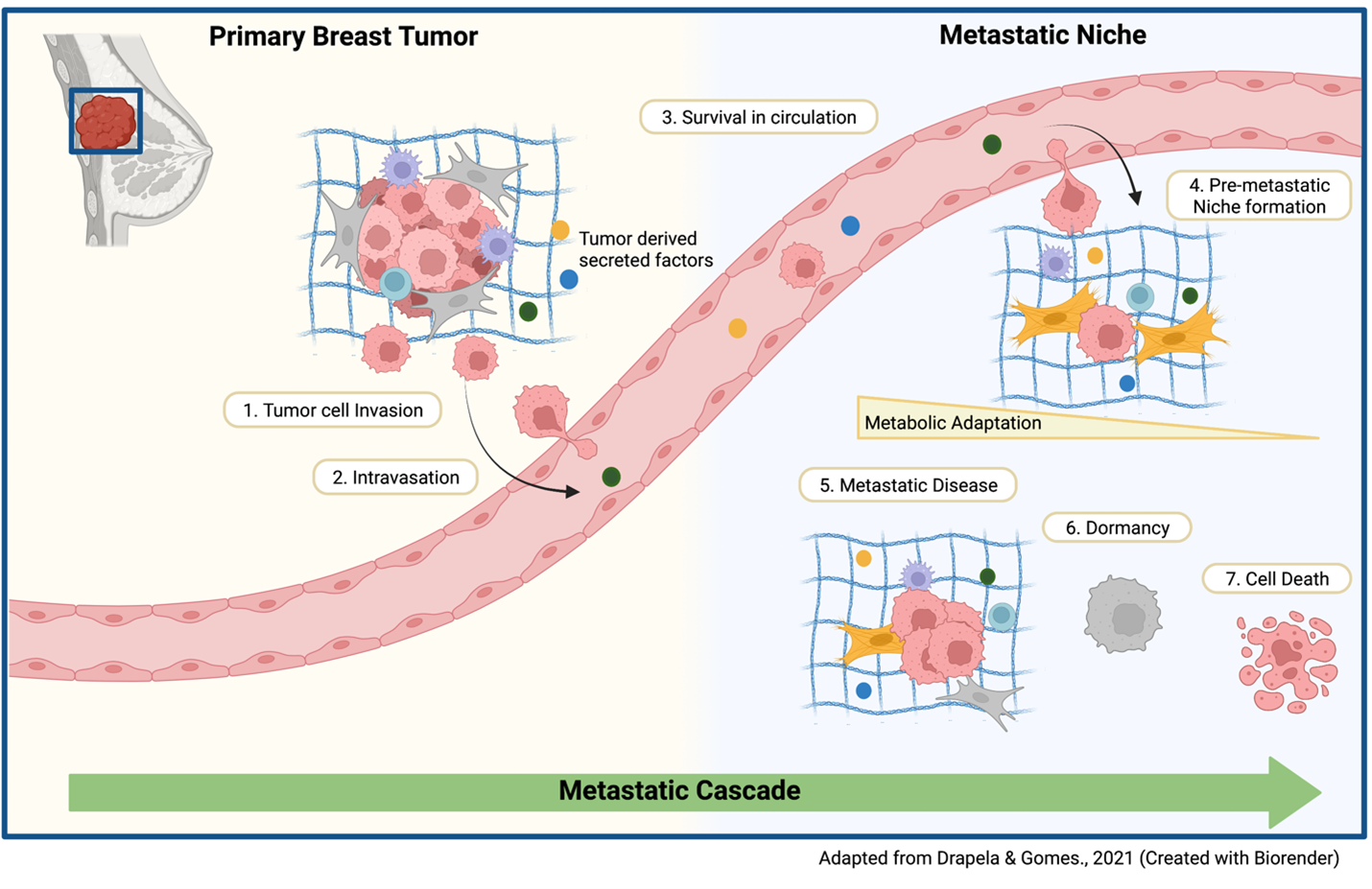
Figure 1: The metastatic cascade. As a primary tumor grows, tumor derived secreted factors are released that alter the local microenvironment making it possible for tumor cells to invade further into tissue outside the tumour. Eventually these tumor cells will reach a blood vessel where they get into circulation until they reach a new environment; if this was been primed for their arrival by such tumor derived factors to favor their growth, it is termed the pre-metastatic niche. The tumor cells will exit the blood vessels into this pre-metastatic niche; they will only survive and grow into secondary tumours if they can metabolically adapt: using adequate nutrients within a space that is very different from the breast, where they are from. The ability of the tumour cell to adapt dictates its fate: proliferate and form secondary tumours, remain dormant or perish. My project aims to understand which processes and cells are involved in these adaptations.
My research focuses on these activated perivascular cells and how they support tumor cells in the lung, by precisely altering tumor cell metabolism and facilitating the formation of lung metastasis.
To address this question, I investigate the interaction between perivascular cells (pericytes) and triple negative breast cancer tumor cells by growing them together (called co-culture assays) to determine how the pericytes might change the metabolic reprogramming of the tumour cells (Figure 2).
Using techniques such as fluorescence imaging, I can see that, when in co-culture, pericytes extend and reach out to tumor cells, sending signals that promote their proliferation. Interestingly, the pericytes also start dividing more, and this suggests that the conversation between the two types of cells results in a co-operative growth advantage to both.
Using metabolic assays that look at the two main energy producing pathways of the cell, glycolysis and oxidative phosphorylation, we see that tumor cells also show altered metabolic activity when they are in the presence of activated pericytes.
So far, our data suggests that pericytes may aid in tumor cell growth at early stages after the tumour cells arrive in the lung, potentially facilitating progression to metastasis in this organ.
By investigating how tumor cells benefit from interactions with pericytes in an early metastatic environment we hope to identify therapeutic opportunities or targets that will reduce the risk of metastatic disease in breast cancer patients.
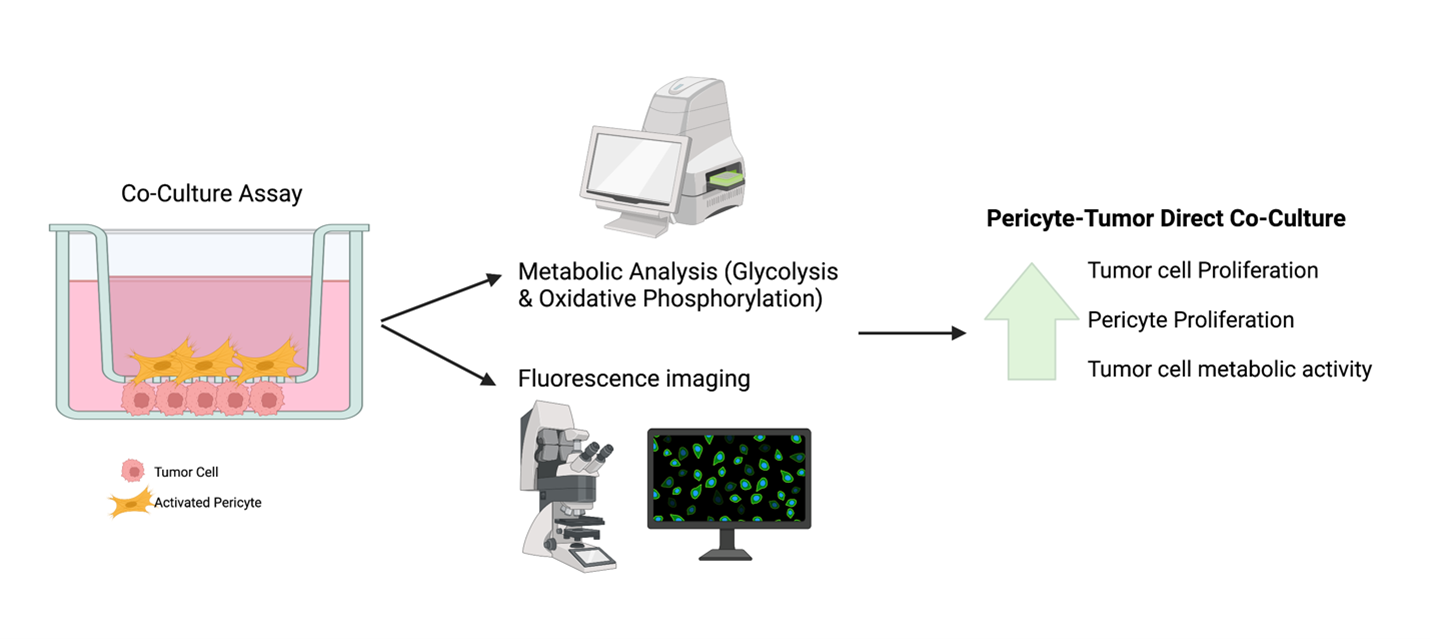
Figure 2: Co-culture experimental design. Direct pericyte-tumor cell interaction increased proliferation in both cell populations suggesting that pericytes and tumor cells reciprocally benefit from each other. We can monitor proliferation in co-culture using live cell imaging with fluorescently labelled cells or immunocytochemistry. Additionally, the cells from co-culture can be used to investigate changes in their metabolic activity. The data provided by these techniques and others, supports our hypothesis that pericytes alter tumor cell metabolism.
