Meet the Experts

Dr Emma Allott
Dr Emma Allott’s research is focused on integrating molecular and epidemiology approaches to identify risk factors for prostate cancer as well as the contributing mechanisms. One current area of research, funded by the World Cancer Research Fund, studies the relationship between periprostatic adipose tissue – a type of fat surrounding the prostate - and aggressive prostate cancer risk. It is known that excess fat surrounding internal organs can be harmful to health. The prostate is no exception in being enveloped by a layer of fat, but the relationship of this so-called periprostatic fat to aggressive prostate cancer risk has never before been tested. More insight into the relationship between periprostatic fat and aggressive prostate cancer could lead to intervention studies and, ultimately, will inform future policies to prevent aggressive prostate cancer. This work has shown that increased quantity of periprostatic fat is found in men with more aggressive prostate tumours, and that the biology of these tumours is distinct from those surrounded by lower amounts of fat.
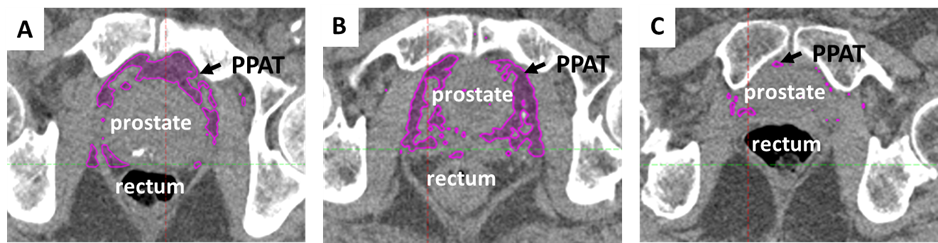
Illustration of the medical imaging-based methods used to measure the quantity of fat surrounding the prostate (periprostatic adipose tissue or PPAT, coloured in pink), in three different men. Notable is the pronounced variation in the amount of this fat type between individuals.
Dr Allott is also seeking to identify factors predicting aggressive and fatal prostate cancer that could be measured at the time of diagnosis, to better inform treatment plans and outcomes. While survival rates for prostate cancer are relatively high overall, a subset of men will die from their disease and this number is predicted to increase substantially in the coming decades. The major challenge lies in identifying men with potentially fatal prostate cancer at diagnosis, so that clinical management can be tailored to maximise treatment success. On the flip side, it is also critical to identify men unlikely to die from their disease, as they could potentially be actively monitored instead of immediately treated, and avoid unnecessary therapeutics and associated side effects in those patients.
Currently, tumour grade is the best predictor of prostate cancer outcomes, and this determined by a pathologist’s assessment based on tumour appearance or morphology. However, it is widely recognized that there are tumour image features invisible to even the best trained, most experienced human eye. Computer ‘vision’, often referred to as artificial intelligence, can be trained to identify these image features. Supported by funding from the Royal Society, Dr Allott's group are using artificial intelligence to identify features of tumour morphology – the appearance of the tumour cells under a microscope - that are unique to men who go on to develop fatal prostate cancer.
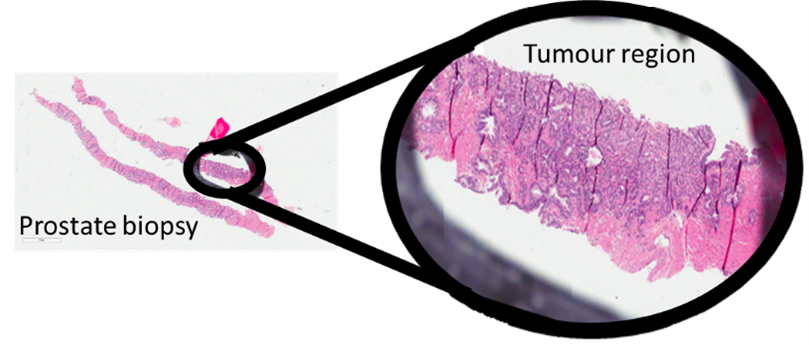
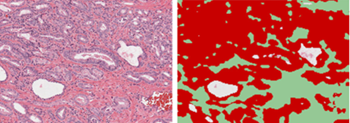
Regions of tumour are identified in diagnostic biopsies by a pathologist, and subsequently subjected to processing by artificial intelligence software to identify features of the tissue that are predictive of fatal outcomes in patients.
Ongoing work in the Allott group seeks to identify the mechanisms leading to improved prostate cancer outcomes in users of the cholesterol-lowering statin drugs. Statins are some of the most commonly used drugs, with approximately half of all men newly diagnosed with prostate cancer using statins. Men using statins have been reported to have a lower risk of developing an aggressive or fatal prostate cancer, and those using statins after diagnosis are more likely to experience better outcomes. However, the mechanisms driving these effects have not been identified. Using clinical data from prostate cancer patients, together with molecular data obtained from corresponding tumour tissue, Dr Allott’s group seek to understand the underlying tumour biology behind this relationship.
