Screening 500,000 drug combinations
Thanks to our innovative drug screening and dispensing technology, Queen’s researchers have the capability to act quickly to test a large number of existing drugs for activity against SARS-CoV2, the virus responsible for COVID-19 disease.
Following the announcement that Queen’s has been awarded a UK Research and Innovation/National Institute for Health Research grant of close to £300,000 to help find a treatment for COVID-19, our haematology experts in The Patrick G Johnston Centre for Cancer Research will be utilising the latest drug screening technology to select suitable anti-viral and anti-inflammatory drugs to test against the disease.
The selected drugs will be tested in models of human lung tissue infected with the SARS-CoV2– the virus that causes the COVID-19 disease – by world-leading virologist Professor Ultan Power and his team at the Wellcome-Wolfson Institute for Experimental Medicine.
The research project aims to screen around 1,000 drugs which are already approved for clinical use in patients with other diseases by the Food and Drug Administration (FDA), the US medicines regulator. Many of the drugs were originally designed to target leukaemia, while others have been tested against other coronaviruses such as SARS (severe acute respiratory syndrome) and MERS (Middle East Respiratory Syndrome). Using smart drug-screening technology, each drug will be selected for testing based on its anti-viral or anti-inflammatory activity.
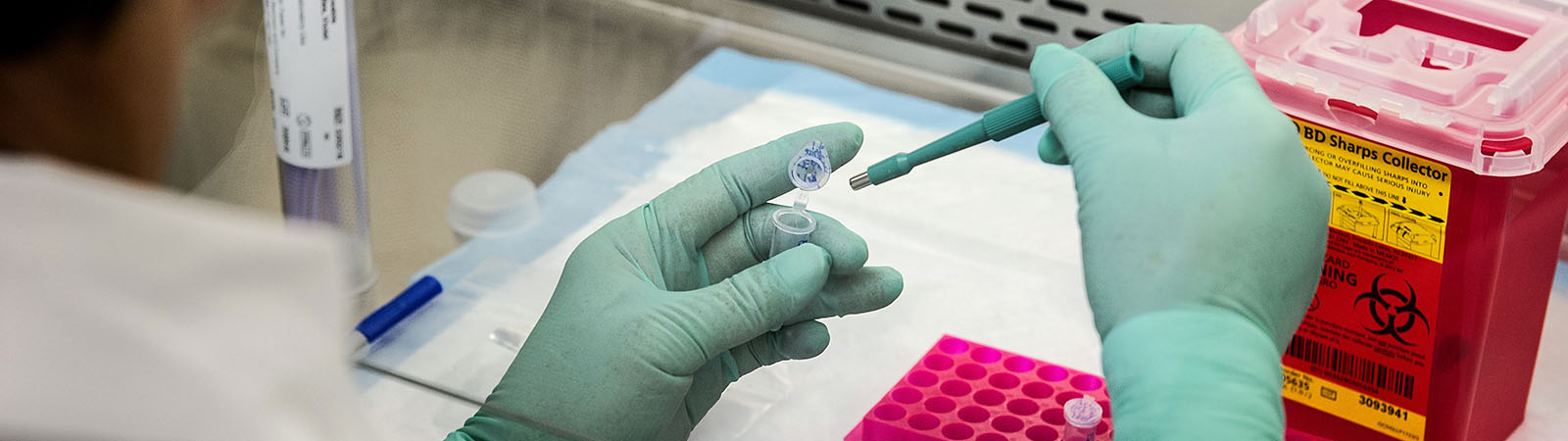
Finding the right combination
While anti-viral drugs could have the potential to inactivate the COVID-19 virus; anti-inflammatory drugs could be the key to dampening down the serious and potentially fatal inflammatory response to the virus that have been seen in certain infected patients around the world. (According to data from the Chinese Centre for Disease Control and Prevention, around 5 per cent of patients in China developed respiratory failure, septic shock, and/or multi-organ failure).
“If the inflammatory response to the COVID-19 virus is too severe, it will send the patient’s immune system into overdrive, causing a tremendous amount of damage to the lungs,” explains Professor Power.
When infection from SARS-CoV2 proceeds down into the lower respiratory tract and into the alveoli (membranous balloon-like structures situated at the end of your respiratory tract), the inflammatory response can starve your body of oxygen and result in respiratory failure.
“This massive inflammatory response can cause damage related directly to these alveoli, as immune cells are summoned to the lungs to try and cope with the infection. The result is pneumonia and a lot of damage to the lung tissues. Part or all of the lungs become non-functional and the patient will go into respiratory failure and die.” says Professor Power.
“Our goal is to try and identify drugs that will prevent this from happening and stop patients reaching this severe stage.”
It’s hoped that when anti-viral and anti-inflammatory drug forces are combined, we might unlock an effective combination that is able to block the SARS-CoV2 virus and mitigate the deadly inflammation that can occur as a result of the COVID-19 disease.

High-tech screening process
With a bank of hundreds of thousands of potential drugs to screen, narrowing down the right combination could potentially be a time-consuming and expensive task. However, in our blood cancer research lab, led by Professor Ken Mills, a co-applicant on the UKRI/NIHR grant, we have evolved technology known as “multiplex screening for interacting compounds” (MuSIC) that has the ability to scan a ‘library’ of drugs quickly and efficiently and at a lower cost.
This technology will allow our researchers to quickly scan over 500,000 potential combinations of drugs to select a shortlist of 1,000 drugs approved for testing by the Food and Drug Administration (FDA), the US medicines regulator.
Dr Ahlam Ali, a Senior Researcher on the project, has a vast amount of experience working with smart drug dispensing and screening systems, including on a recent project developing a Human Papilloma Virus (HPV) vaccine. “My expertise is in drug discovery and drug delivery,” she says. “For this project, I am now going to be focussing my skills on drug repurposing for COVID-19.”
Dr Ali adds, “MuSIC will significantly speed up the screening process and reduce the cost.”
Rapid and precise dispensing
Once the drugs have been selected for testing, a rapid and precise dispensing method is required to ensure accurate measures and limit any wastage. Dr Ali and her team are working with Queen’s Genomics Core Technology Unit to utilise a robotic liquid dispensing handler called Echo.
This machine offers tip-less, non-contact liquid transfer that is rapid, robust and precise, ultimately improving our data quality and increasing the potential to find new therapeutics.
“We have lots of experience of using the Echo machine,” says Dr Ali. “We are currently using it to screen for different drugs to potentially treat paediatric acute myeloid leukaemia (AML).
“Echo will offer quick and precise distribution of the drug which will ultimately speed up the drug-screening process,” she explains.